Insurance denial rates increased in 2025
April 14, 2026
Summary: A 2025 revenue cycle report found that provider revenue losses from denials and bad debt increased from 2024, and patients paid a smaller share of their out-of-pocket responsibility.
Source: Szaflaski, M State of Health Care Revenue Cycle Kodiak Solutions, March 30, 2026
Providers often complain about the rate of insurer denials, while insurers point out that many denials are due to billing errors, including duplicates or incorrect information submitted. While federal regulations require health plans to report denial rates for Medicare Advantage, no equivalent requirement exists for commercial insurance, making current data difficult to obtain.
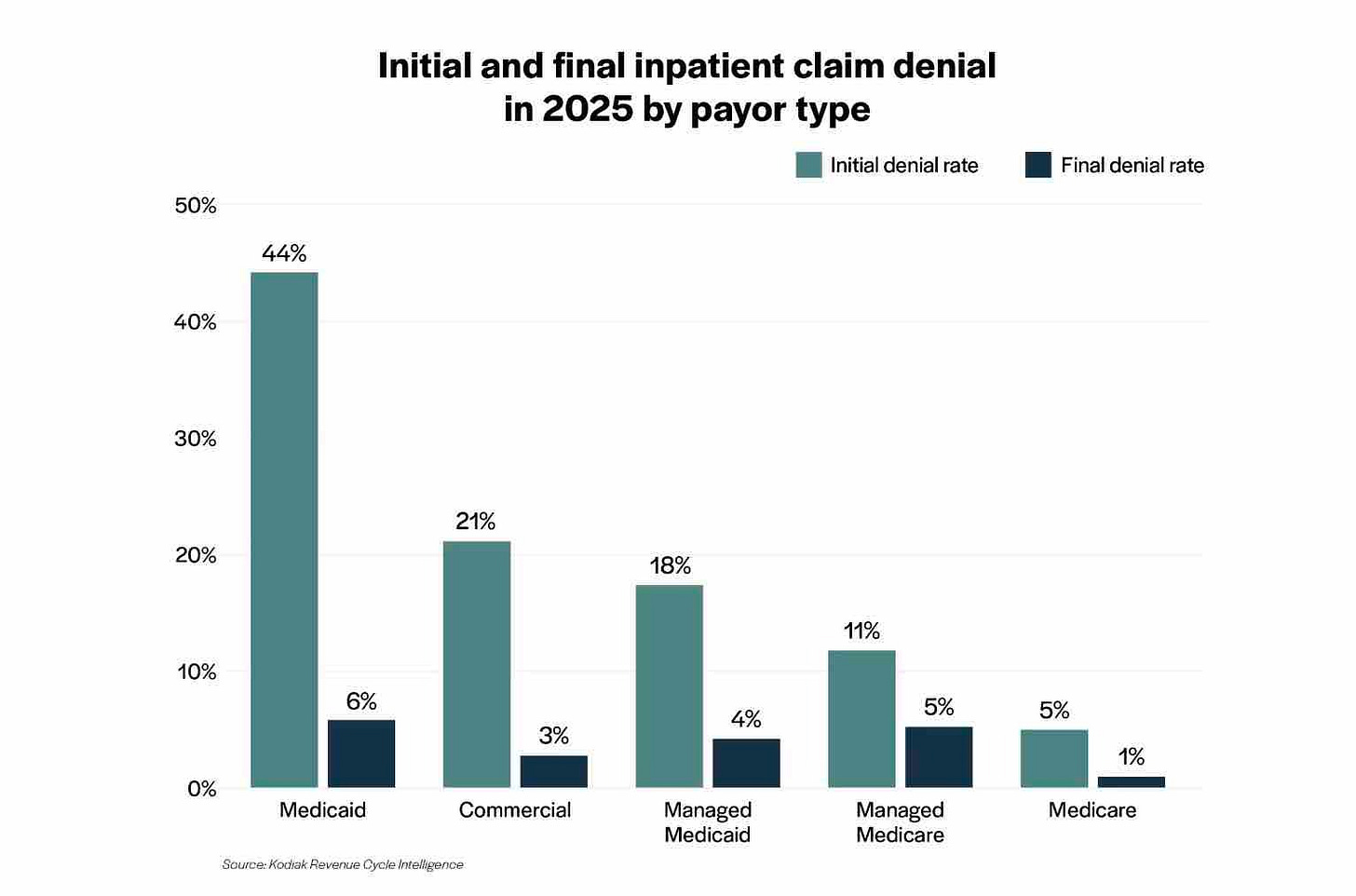
A report from Kodiak Solutions, a revenue cycle consultancy, provided 2025 data on inpatient and outpatient claims denials from its clients. It found that 21% of inpatient claims in the commercial population were initially denied, although the final denial rate was only 3%. Eleven percent of outpatient claims were denied, and the final denial rate was also 3%. A process in which so many denials are eventually overturned is in serious need of reform. Kodiak also found that out-of-pocket responsibility increased from 6.8% to 7.3%, and reported a decrease in the “insured patient yield,” the percentage of billed out-of-pocket amounts actually collected from patients. Overall loss of provider revenue due to denial rates and bad debt increased from 2024 to 2025.
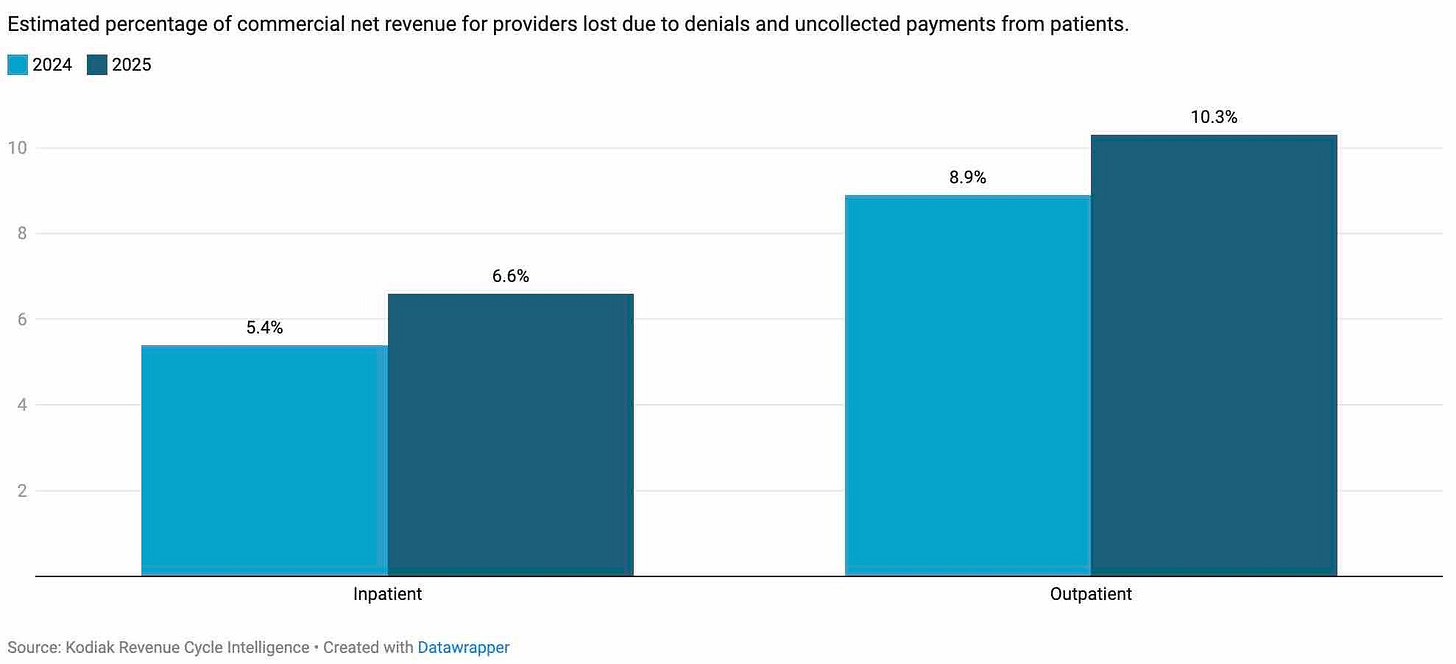
Provider revenue loss due to denials and bad debt
Source: Kasic, et al Rising claims denials dent provider revenue Modern Healthcare, April 6, 2026
Implications for employers:
Insurer denials represent a pain point for both patients and providers, and add unnecessary administrative burden and costs.
Employers can ask their carrier for their denial ‘cascade,’ from initial denials to final denials. If that gap is high, then employers can ask their carrier what they are doing to better adjudicate these denials.
Employers can expect denials and payment policies to continue to be factors in provider-plan contract negotiations.
Insurers that meaningfully reduce denial friction could secure more favorable provider contracts, although eliminating prior authorization and utilization management altogether risks increased total costs.
Tomorrow: Are insurance plans really reducing prior authorization?